How to Leverage AI in Healthcare: Top 8 Applications
- Introduction
- AI in Medical Imaging
- Predictive Analytics for Patient Care
- Personalized Medicine through AI
- 4. Chatbots and Virtual Health Assistants
- Drug Discovery and Development
- Remote Patient Monitoring
- AI in Clinical Decision Support Systems (CDSS)
- Enhancing Medical Research with AI
- Challenges and Ethical Considerations
Introduction
Artificial intelligence (AI) has emerged as a pivotal force in the transformation of healthcare, revolutionizing the way medical practitioners approach diagnosis, treatment, and patient management. The integration of AI-driven technologies into clinical settings is altering traditional practices and improving the efficiency and accuracy of patient care. As healthcare systems face the challenges of an aging population, increasing patient volumes, and the necessity for personalized medicine, the reliance on AI solutions continues to grow.
One significant impact of AI in healthcare is its ability to process vast amounts of data at astonishing speeds. This capability allows healthcare providers to make informed decisions based on real-time analytics and predictive modeling, ultimately leading to better patient outcomes. From assisting in diagnosis to recommending personalized treatment plans, AI technologies are proving essential in the clinical decision-making process.
Moreover, the applications of AI are diverse, encompassing various domains such as medical imaging, genomics, drug discovery, and telemedicine. Each of these areas benefits from AI’s enhanced analytical capabilities, facilitating advancements that were previously deemed unattainable. For instance, AI algorithms can analyze medical images with precision comparable to that of expert radiologists, enabling earlier detection of conditions and facilitating timely intervention.
As we delve into the specifics of the top ten applications of AI in healthcare, we will explore how these innovations are not only streamlining operations but are also fundamentally redefining the patient experience. The growing synergy between AI technologies and clinical practices represents a significant leap forward in the pursuit of efficient, effective, and accessible healthcare for all.
AI in Medical Imaging
Artificial Intelligence (AI) is revolutionizing the field of medical imaging, significantly enhancing the capabilities of image analysis. Through sophisticated algorithms and deep learning techniques, AI applications facilitate the faster and more accurate diagnosis of various medical conditions. These advancements are particularly crucial in radiology, where timely and precise interpretation of images can greatly impact patient outcomes.
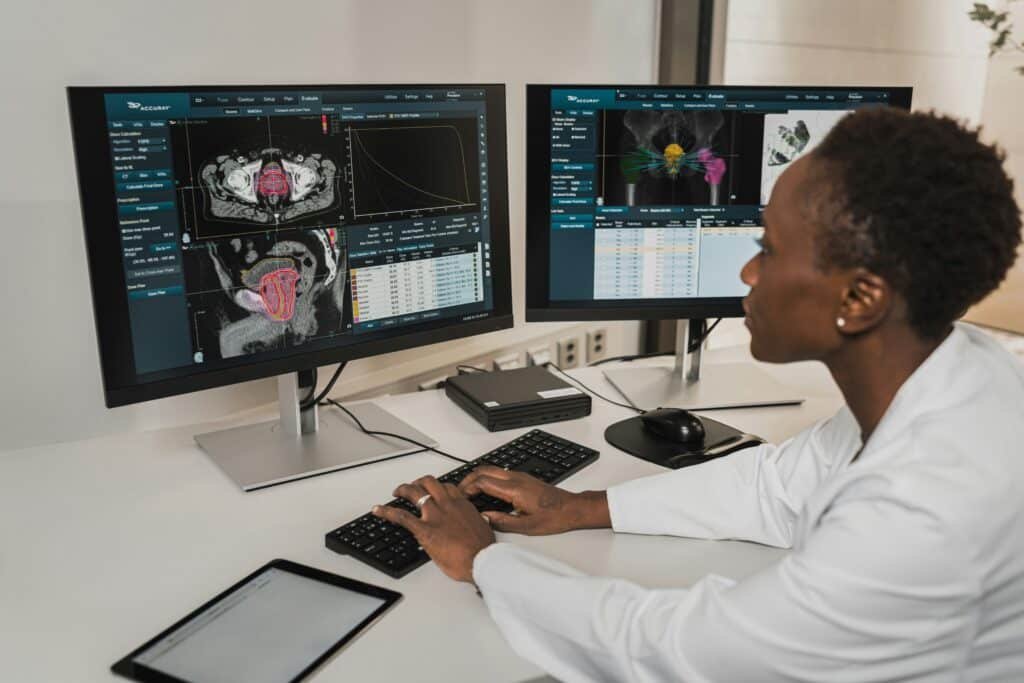
One key area of AI’s application in medical imaging is the analysis of X-rays, CT scans, and MRIs. AI systems are designed to identify patterns and anomalies in images that may not be immediately apparent to the human eye. For instance, deep learning algorithms developed by companies such as Zebra Medical Vision and Aidoc can detect abnormalities in imaging studies, from fractures to tumors, more swiftly than traditional methods. These tools not only speed up the diagnostic process but also reduce the workload on radiologists, allowing them to focus on complex cases that require human expertise.
Numerous studies have documented the effectiveness of AI in improving diagnostic accuracy. For example, a recent study published in “Nature” showcased an AI model that outperformed experienced radiologists in detecting breast cancer in mammograms. Similarly, research in the “Journal of the American College of Radiology” highlighted that AI-assisted imaging interpretation could lead to better identification rates of lung nodules, therefore enabling earlier interventions.
The integration of AI in medical imaging also promotes consistency and reduces variations in interpretations, addressing a common challenge in the field. As healthcare continues to evolve, the collaboration between AI and human professionals is expected to play a vital role in advancing medical diagnostic capabilities, ultimately enhancing patient safety and care.
Predictive Analytics for Patient Care
Predictive analytics in healthcare refers to the use of statistical techniques, algorithms, and machine learning approaches that analyze current and historical patient data to identify potential health events. The utilization of artificial intelligence (AI) in predictive analytics is transforming the landscape of patient care by enabling healthcare providers to forecast and mitigate risks, thereby leading to improved patient outcomes.
AI models employ vast datasets, which may include patient demographics, medical histories, lab results, and even social determinants of health, to detect patterns that could indicate imminent health complications. By leveraging these data points, predictive analytics can inform clinicians whether a patient may develop conditions such as diabetes, heart disease, or other chronic illnesses. For instance, an AI system might analyze a patient’s data and flag an increased risk of heart failure, prompting proactive measures from healthcare providers.
Several case studies highlight the successes of AI in predictive analytics within healthcare settings. One notable example is the use of AI algorithms by healthcare institutions to predict patient readmission rates. By analyzing factors such as previous hospital visits and vital signs, specific AI models have effectively reduced readmissions by 20%, allowing for targeted preventive care. Another case study from a large healthcare provider demonstrated how their AI-driven analytics platform accurately predicted sepsis onset in patients, enabling earlier intervention and decreasing mortality rates.
As predictive analytics continues to evolve with advancements in AI, its potential to enhance patient care becomes increasingly evident. AI not only facilitates the identification of at-risk patients but also empowers healthcare professionals to implement preventive strategies, ultimately leading to more effective healthcare delivery. Through the integration of AI in predictive analytics, healthcare systems can move toward a more proactive and personalized approach to patient care.
Personalized Medicine through AI
The incorporation of artificial intelligence (AI) into healthcare is significantly transforming the concept of personalized medicine. By utilizing advanced algorithms, AI can assess a multitude of data, from genetic information and lifestyle habits to previous treatment outcomes. This comprehensive analysis aids healthcare professionals in developing tailored treatment plans that cater to the specific needs of individual patients.
One of the primary advantages of personalized medicine powered by AI is its potential to enhance treatment efficacy. For instance, platforms like IBM Watson Health leverage AI to analyze vast datasets, providing insights that enable clinicians to select therapies based on patients’ unique genetic profiles. Such an approach not only improves treatment success rates but also minimizes the risk of adverse effects, as therapies are fine-tuned to align with each patient’s molecular and phenotypic characteristics.
AI also allows for the dynamic adjustment of treatment plans over time. Continuous monitoring and data collection ensure that insights generated from ongoing treatments can inform future decisions. One notable example is Tempus, a technology company that uses AI to interpret clinical and molecular data, streamlining the process of matching patients with appropriate therapies. By integrating real-world evidence with genomic data, Tempus contributes to more precisely directed medical strategies.
In summary, AI’s role in personalized medicine represents a paradigm shift in how medical professionals can approach treatment. By tailoring therapies based on detailed patient profiles, AI empowers healthcare providers to deliver more effective and safer treatments, ultimately advancing the overall quality of care.
4. Chatbots and Virtual Health Assistants
Chatbots and virtual health assistants have emerged as pivotal tools within the healthcare landscape, serving to enhance patient engagement and streamline communication between healthcare providers and patients. These AI applications utilize advanced natural language processing algorithms to interpret and respond to patient inquiries, thereby providing immediate answers to health-related questions. This immediacy not only empowers patients with instant access to information but also alleviates the workload of healthcare professionals, allowing them to devote more time to complex cases.
The deployment of chatbots allows healthcare facilities to maintain a 24/7 operational presence, ensuring patients receive support whenever needed. By integrating symptom-checking functionalities, these AI-powered systems can assist in triaging patients effectively. When patients present with symptoms, the virtual assistants can evaluate their conditions based on inputs received and guide them on the appropriate next steps, which can include scheduling an appointment with a physician or suggesting over-the-counter remedies.
The technology underpinning these chatbots is continually evolving. Machine learning models are trained on vast datasets, enabling these systems to provide increasingly accurate responses to various health inquiries. Furthermore, the implementation of AI-based solutions fosters a more personalized patient experience by learning individual preferences and health histories. Surveys and feedback mechanisms can also be integrated into these systems, allowing healthcare organizations to assess and enhance patient satisfaction continually. By facilitating improved communication, reducing response times, and offering reliable health information, chatbots and virtual health assistants significantly contribute to an overall better healthcare experience for patients.
Drug Discovery and Development
The field of drug discovery and development has undergone significant transformation due to the integration of artificial intelligence (AI) technologies. Traditionally, drug development is a time-consuming and costly process, involving extensive research, clinical trials, and regulatory compliance. However, AI’s capabilities in data analysis and predictive modeling have simplified the identification of promising drug candidates, enabling pharmaceutical companies to streamline these processes.
AI systems are now utilized to analyze vast datasets, including genetic information, biochemical data, and clinical outcomes. By employing machine learning algorithms, these systems can identify patterns and correlations that may not be evident to human researchers. This predictive power allows for the rapid screening of potential compounds, effectively narrowing down a plethora of candidates to those most likely to succeed in treating specific diseases.
Furthermore, AI enhances the design of clinical trials by predicting the best patient populations and optimal dosing strategies. This helps in minimizing trial failures and maximizing the chances of success. Various platforms harness AI to simulate different trial scenarios, optimizing factors such as participant selection and trial endpoints. As a result, clinical trials can be executed more efficiently, reducing time-to-market for new drugs.
Several notable case studies demonstrate the efficacy of AI in drug development. For instance, Atomwise’s AI platform has been instrumental in identifying candidates for diseases like Ebola and multiple sclerosis, significantly shortening the discovery timeline. Similarly, insilico Medicine used deep learning to discover a novel drug for fibrosis, beginning with the initial compound to its refinement in just a few days. Such innovations underscore the indispensable role that AI plays in accelerating drug discovery and development, fundamentally improving pharmaceutical outcomes and cost-effectiveness.
Remote Patient Monitoring
Remote patient monitoring (RPM) has emerged as a transformative application of artificial intelligence in healthcare, making it possible to observe and manage patients’ health from a distance. This innovation is largely driven by wearable devices and IoT (Internet of Things) technologies, which facilitate continuous health monitoring. By collecting real-time data on various health metrics, such as heart rate, blood pressure, and glucose levels, these AI-powered solutions enable healthcare providers to accurately assess a patient’s condition without the need for constant in-person visits.
One significant advantage of RPM is its potential for proactive management of chronic diseases. For patients suffering from conditions like diabetes or heart disease, timely insights derived from monitored data allow healthcare professionals to make informed decisions and intervene when necessary. These interventions can range from medication adjustments to lifestyle recommendations, significantly enhancing patient outcomes and quality of life.
However, implementing remote patient monitoring poses certain challenges. Privacy concerns regarding the sharing of sensitive health data must be addressed, ensuring compliance with regulations such as HIPAA. Moreover, the inconsistent technology adoption among different patient demographics can lead to inequities in access to RPM solutions. While younger, tech-savvy populations may readily embrace wearable devices, older adults, or those less familiar with technology may struggle to engage with these innovations.
Despite these challenges, the benefits of remote patient monitoring cannot be overlooked. It represents a significant advancement towards personalized healthcare, where treatments can be tailored based on real-world data gathered continuously. As AI continues to evolve, the integration of remote patient monitoring into routine healthcare practice will likely become more seamless and effective, paving the way for a more engaged and informed patient population.
AI in Clinical Decision Support Systems (CDSS)
Clinical Decision Support Systems (CDSS) are crucial tools in modern healthcare, leveraging artificial intelligence (AI) to provide healthcare professionals with insightful data that aids in clinical decision-making. These systems analyze extensive datasets, including patient history, lab results, and current medical literature, enabling them to deliver evidence-based recommendations tailored to individual patient needs.
One of the primary advantages of incorporating AI in CDSS is its ability to process and evaluate vast arrays of clinical data rapidly. Traditional methods of analysis can be time-consuming and may lead to inconsistencies, while AI-driven systems can filter through information at a pace that supports timely decision-making. For instance, AI can identify patterns in patient symptoms that might not be immediately recognizable to a clinician, thus enhancing diagnostic accuracy.
Moreover, AI in CDSS promotes adherence to clinical guidelines by offering reminders and alerts when care deviates from evidence-based protocols. This functionality ensures that healthcare providers remain alert to the latest treatments and recommendations, ultimately improving patient outcomes. Best practices for utilizing CDSS effectively include integrating these tools within existing electronic health record systems to provide seamless access to relevant patient data.
However, it is essential to ensure that clinicians maintain active engagement with AI-generated recommendations. While AI can significantly enhance productivity, the final clinical decision should always rest with qualified healthcare providers. The integration of AI in CDSS not only facilitates informed decision-making but also encourages continuous learning and adaptation among healthcare professionals as they confront diverse medical scenarios.
Investing in robust training programs that educate healthcare providers on the optimal use of these systems is also critical. Such initiatives can empower clinicians to make the most of available AI tools, fostering a culture of collaboration between man and machine that ultimately benefits patient care.
Enhancing Medical Research with AI
Artificial Intelligence (AI) is revolutionizing medical research, offering unprecedented tools to analyze, interpret, and derive insights from large datasets. Traditionally, medical research has involved manual analysis of data, which can be time-consuming and prone to human error. However, AI applications can process vast amounts of information at speeds far surpassing those of human researchers. This capability not only enhances efficiency but also significantly accelerates the discovery of new treatments and therapies.
One of the core strengths of AI in medical research lies in its ability to identify underlying trends and patterns within complex datasets. Machine learning algorithms can sift through thousands of clinical trials, research papers, and patient records to highlight correlations that might remain undetected through manual analysis. For instance, AI has proven instrumental in genomics, enabling researchers to analyze DNA sequences to identify genetic markers linked to specific diseases. This has led to breakthroughs in personalized medicine, where treatments are tailored to individuals based on their genetic profiles.
Furthermore, AI systems can facilitate the design of new clinical studies by predicting patient enrollment rates, optimizing protocol design, and determining suitable endpoints. These enhancements not only reduce the time required to initiate research projects but also improve their efficacy. An example can be seen in the development of AI algorithms capable of predicting patient responses to therapies. This predictive capability allows for more precise targeting of interventions, which can lead to quicker progress in clinical trials.
In conclusion, the integration of AI into medical research is transforming the landscape of scientific discoveries. By leveraging its capabilities to analyze extensive datasets swiftly and accurately, researchers can explore new avenues of treatment and expand the understanding of various health conditions, ultimately contributing to better healthcare outcomes.
Challenges and Ethical Considerations
The integration of artificial intelligence (AI) into healthcare presents numerous challenges and ethical considerations that must be thoroughly examined. A primary concern is the privacy and security of patient data. As AI systems rely on vast datasets to enhance their algorithms and improve diagnostic accuracy, they often necessitate access to sensitive medical information. This raises the issue of safeguarding personal data and ensuring compliance with regulations such as the Health Insurance Portability and Accountability Act (HIPAA) in the United States. Health organizations must implement robust data protection measures to maintain patient confidentiality and trust.
Another significant challenge arises from biases inherent within AI algorithms. These biases can stem from unrepresentative training data, leading to inequitable healthcare outcomes across different populations. When AI systems are trained primarily on data from specific demographic groups, they may perform poorly when applied to broader, more diverse populations. Addressing this issue requires ongoing efforts to diversify datasets and refine algorithms to ensure that AI applications are equitable and do not exacerbate existing healthcare disparities.
To navigate these challenges effectively, the establishment of comprehensive regulatory frameworks is essential. Policymakers must collaborate with healthcare professionals, technologists, and ethicists to formulate guidelines that govern the development, deployment, and utilization of AI in healthcare. Ethical frameworks that address accountability, transparency, and fairness in AI applications can help mitigate concerns while fostering innovation. Furthermore, continuous monitoring and evaluation of AI systems will be vital to ensure they operate within ethical boundaries and produce fair outcomes. By adopting these strategies, the healthcare sector can harness the potential of AI while addressing the associated challenges responsibly.

